Recovery After Pneumonia: Stages and Methods of Rehabilitation
Recovery after pneumonia and COVID-19. Stages of medical rehabilitation, electrotherapy/restorative therapy methods, dietary guidelines, and complication prevention.
This article is for informational purposes only
The content on this website, including text, graphics, and other materials, is provided for informational purposes only. It is not intended as advice or guidance. Regarding your specific medical condition or treatment, please consult your healthcare provider.
Hemothorax is an accumulation of blood in the pleural cavity with a ratio of pleural fluid hematocrit to peripheral blood hematocrit of 50% or more.
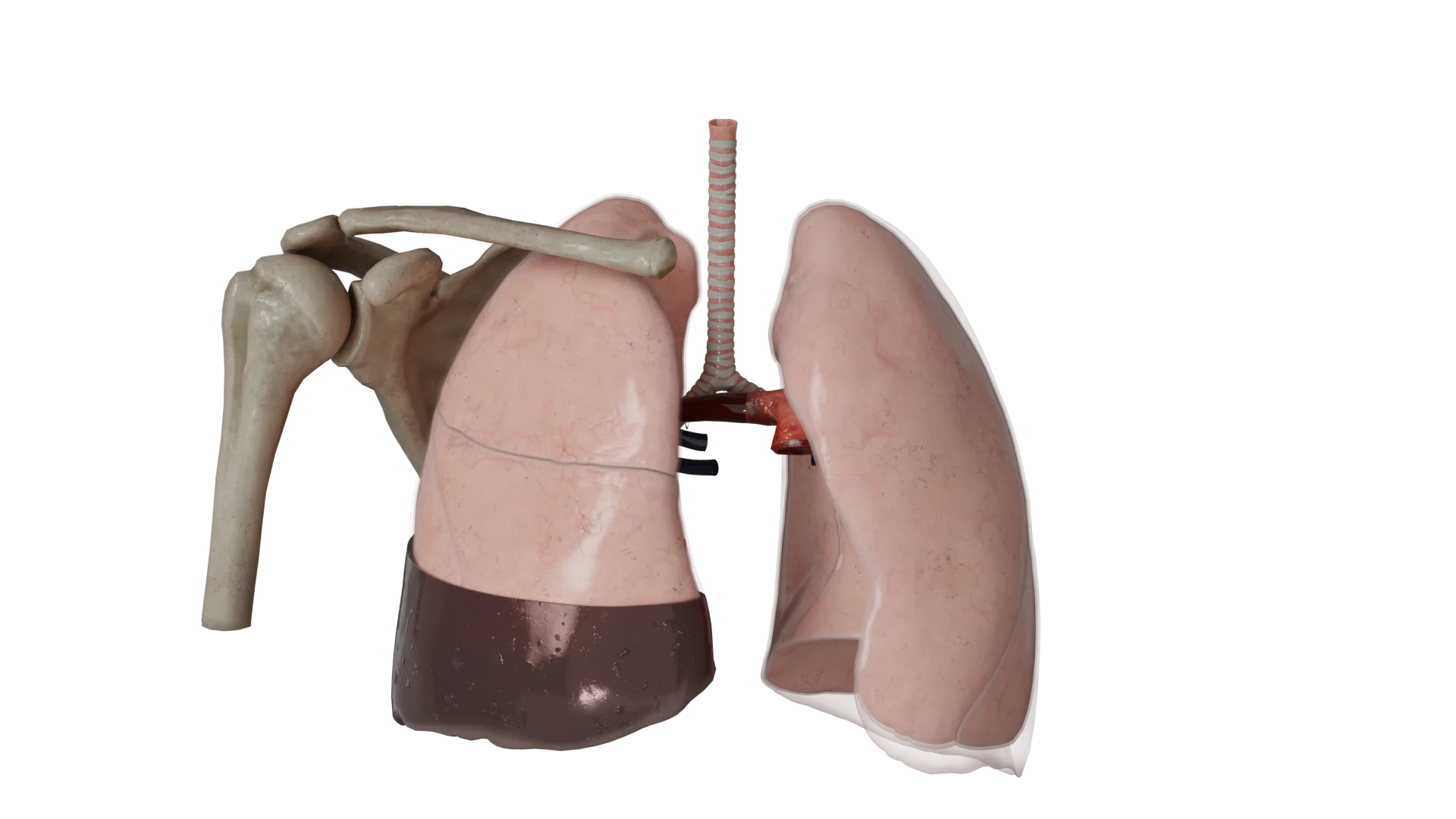

This pathology occurs due to damage of various sizes of arteries and veins of the lung parenchyma, chest wall, mediastinum, diaphragm, etc. The most common cause of hemothorax is chest trauma (non-penetrating, penetrating or iatrogenic). Non-traumatic causes (oncologic diseases, tuberculosis, coagulopathies, etc.) are less common.
In our application models, we consider variants of hemothorax of traumatic genesis.
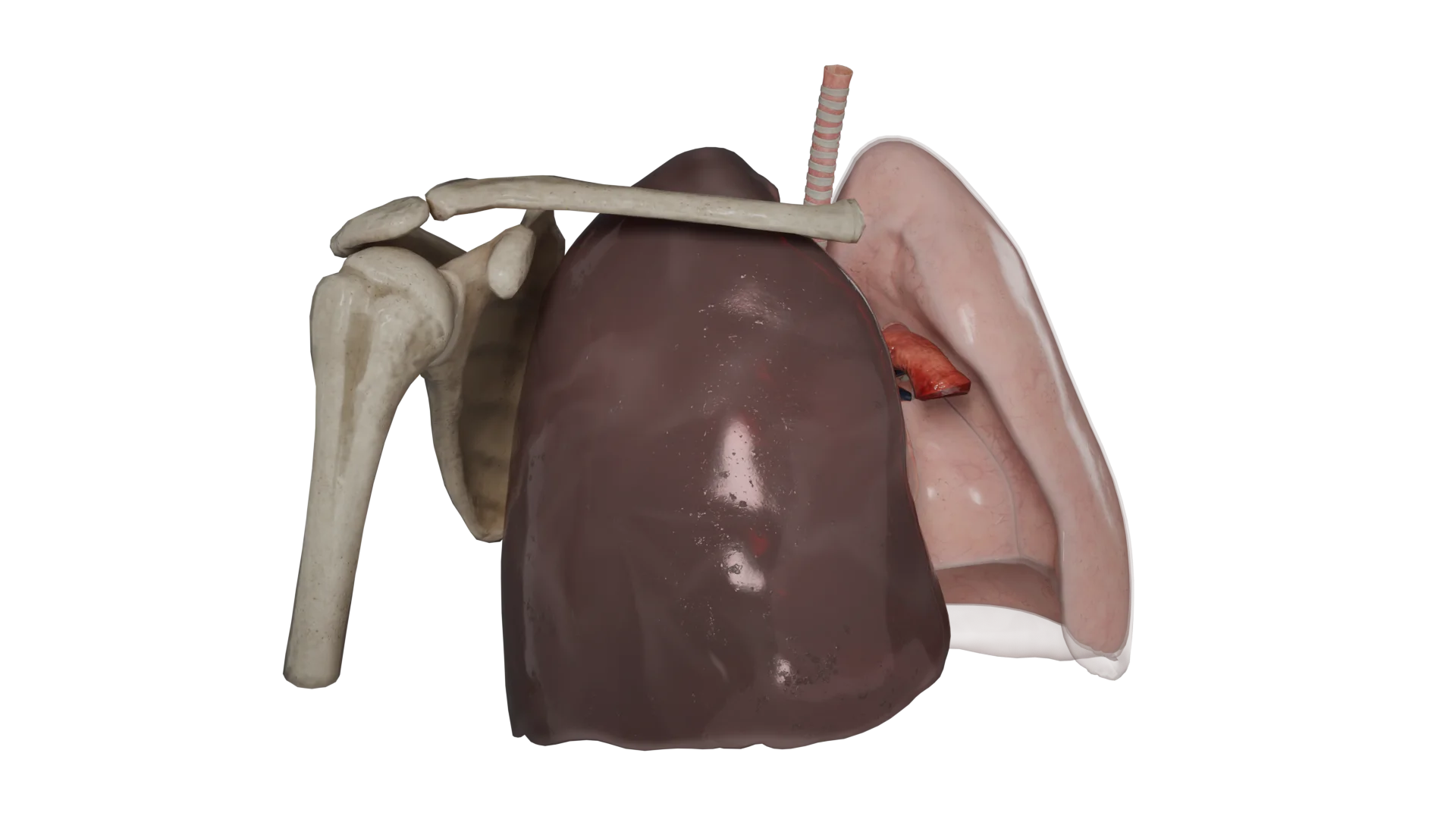
All hemothorax models present a mock-up of a person in the upright position.
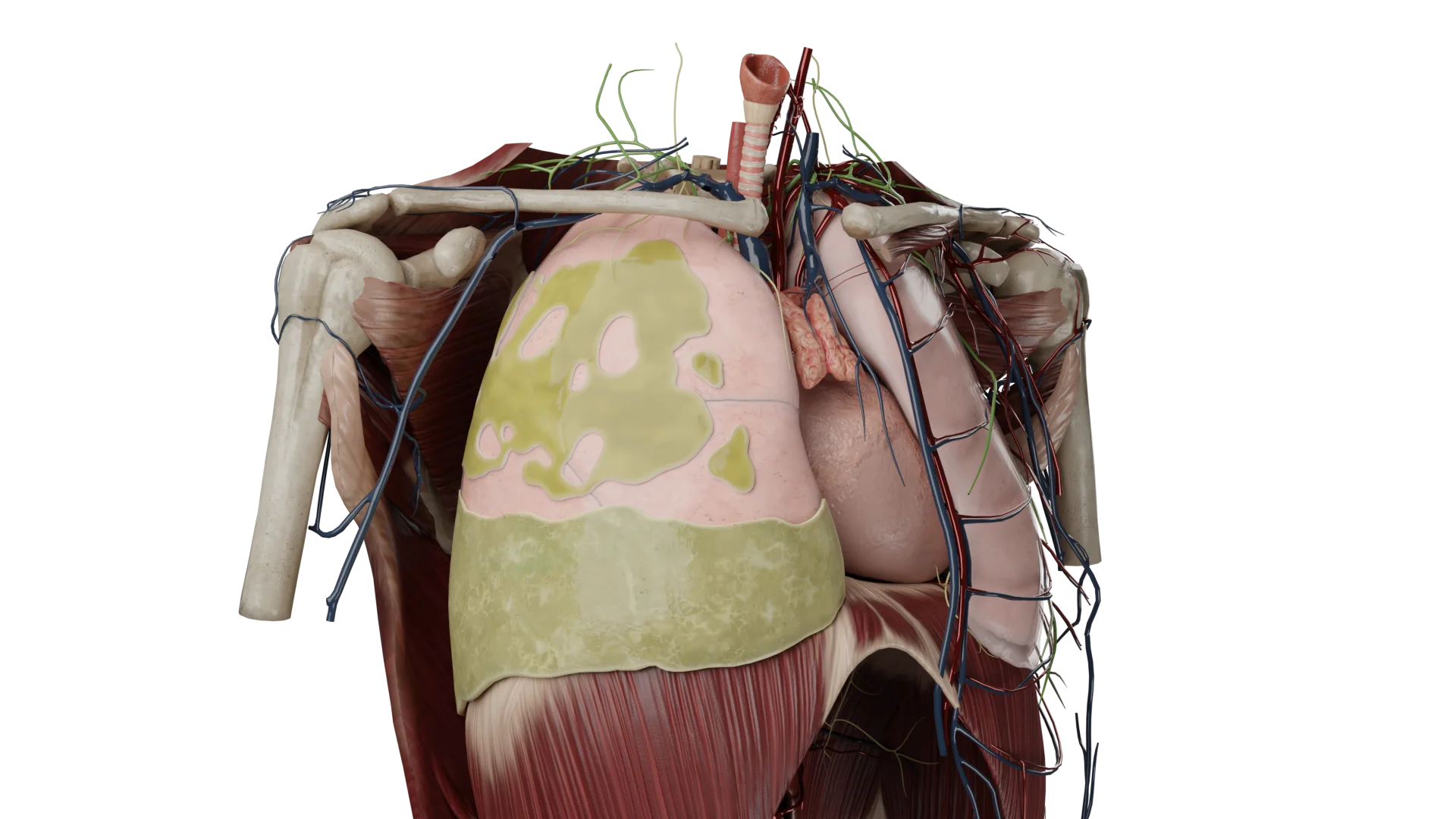
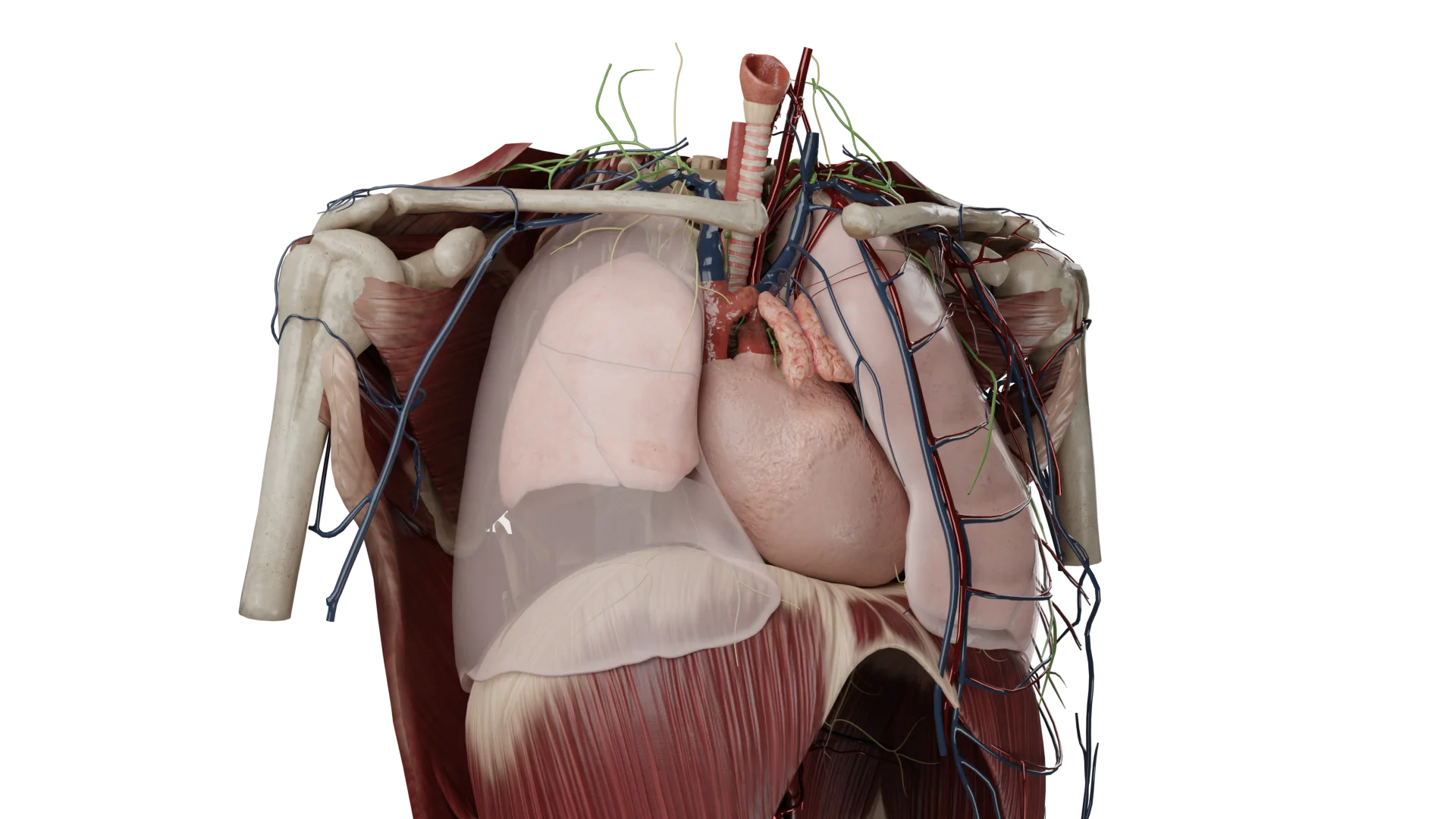
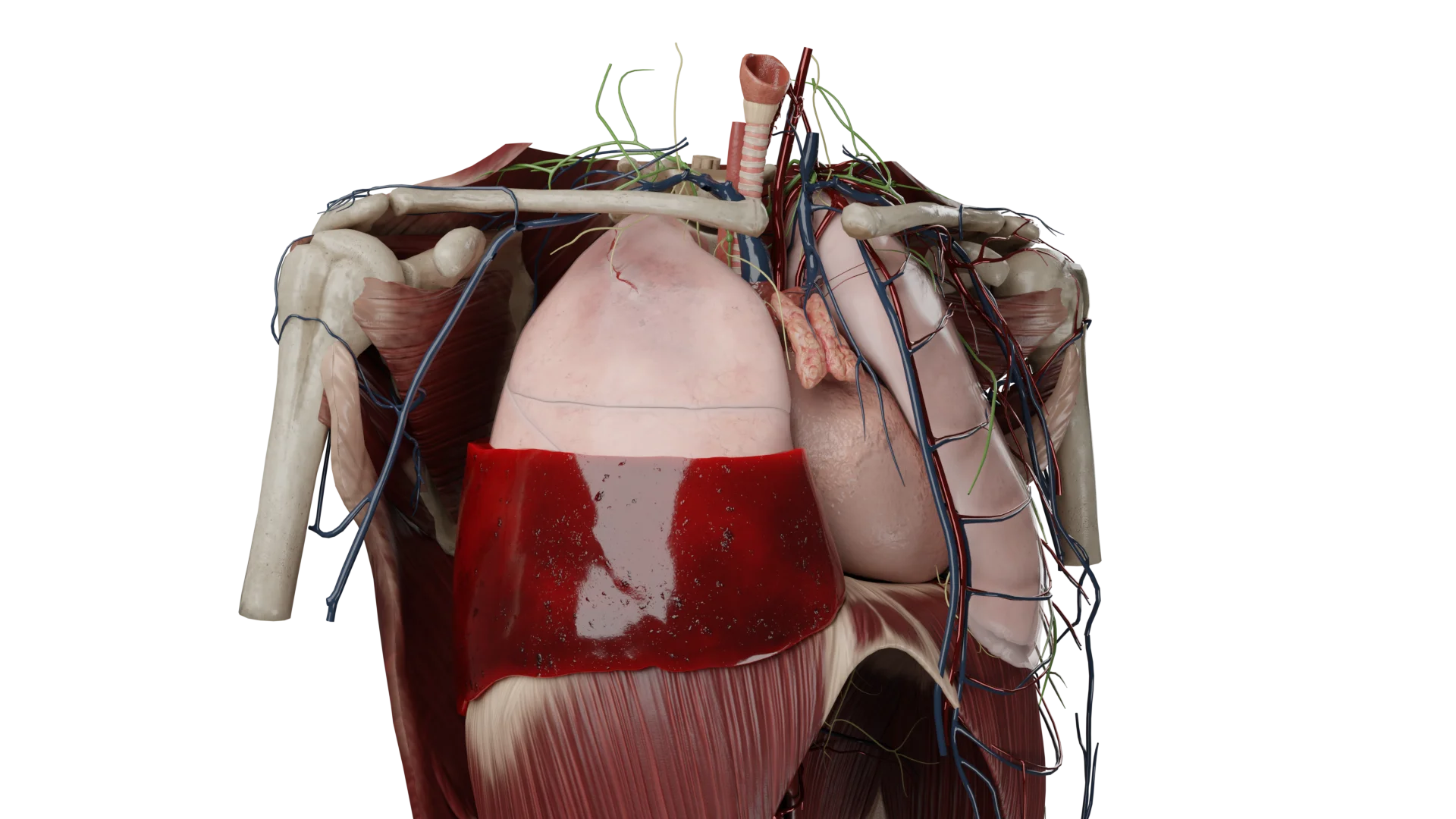
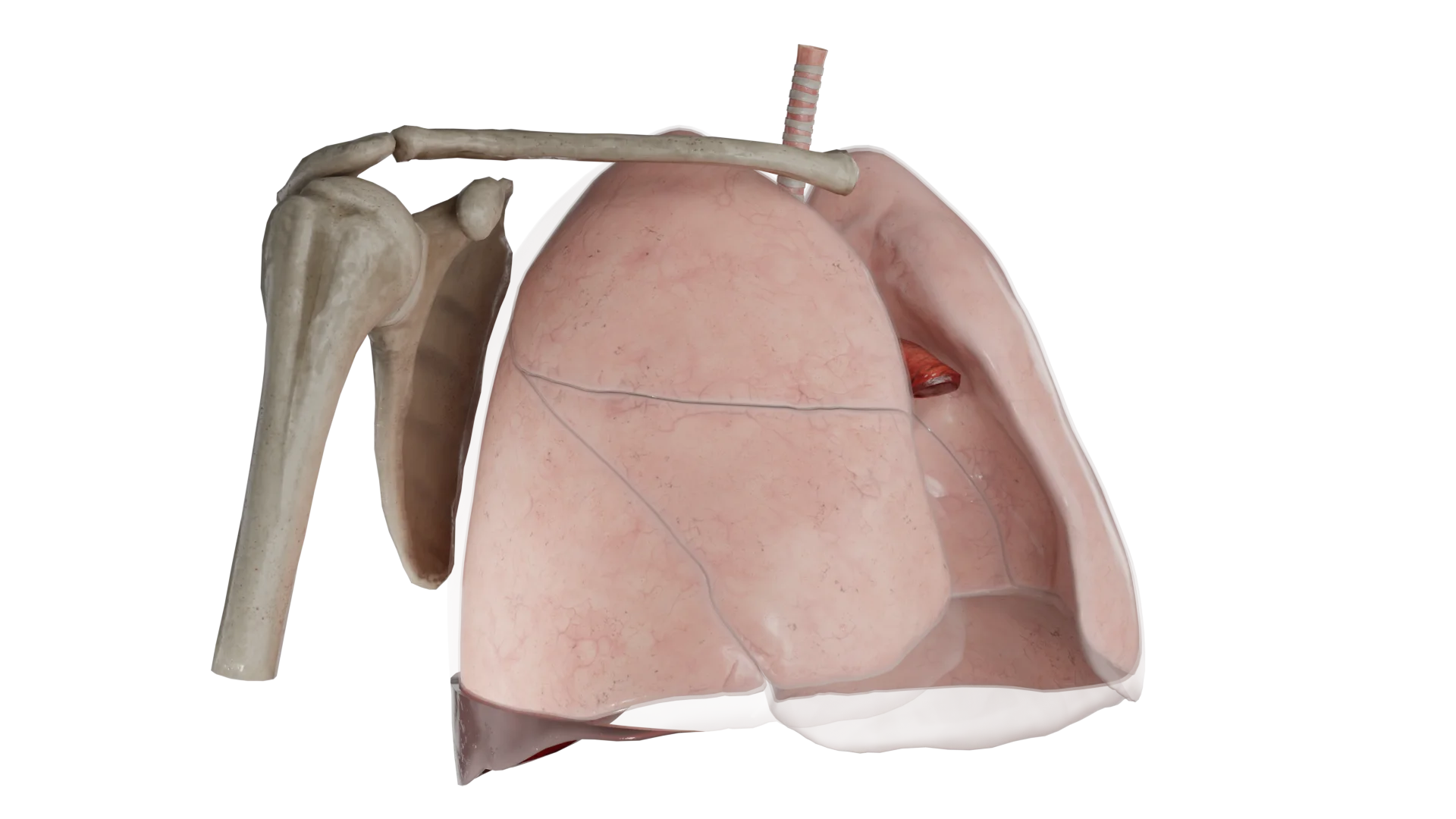
In hemothorax, a horizontal level of fluid can be seen, with a damaged intercostal vessel on the posterior surface of the chest. In moderate and massive hemothoraxes, the volume of blood presses on the lung and collapses it.
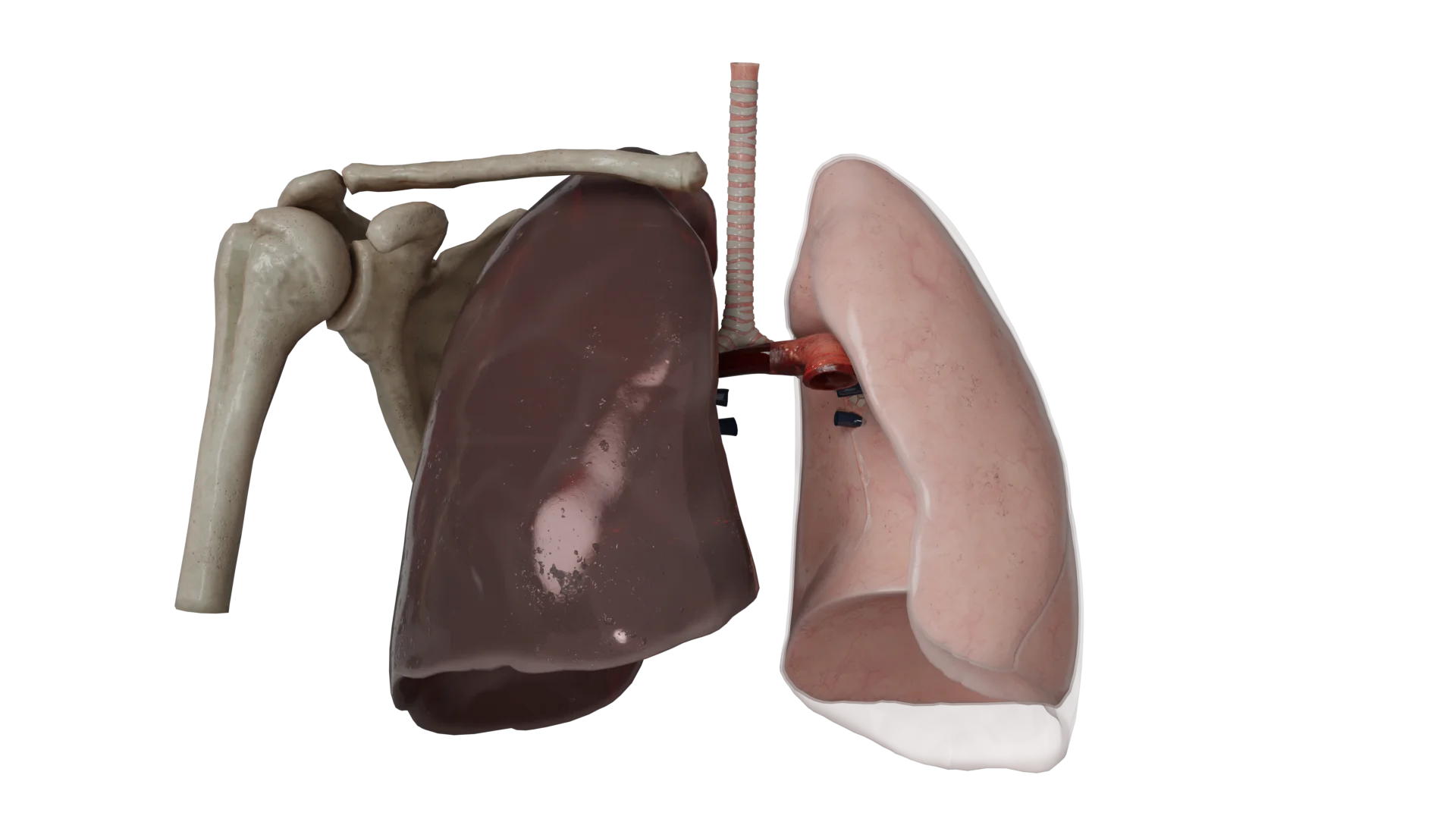

In models of detached hemothorax we see drained blood of various localizations.
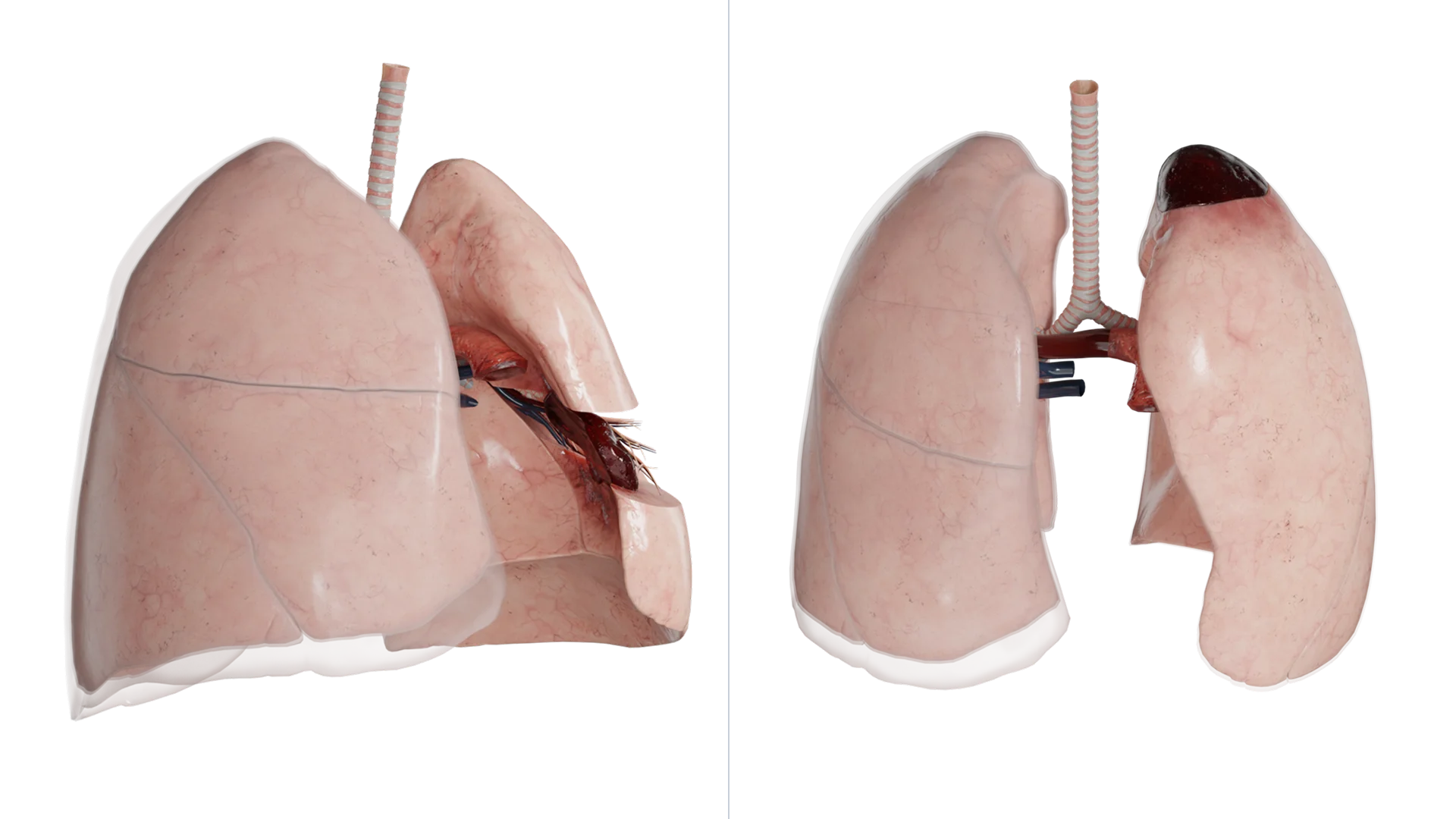

By etiology, they are distinguished:
Hemothorax is classified according to the volume of blood in the free pleural cavity in adults (in children, due to the large amplitude of sex and age differences, it is better to use radiologic classification):
A detached hemothorax happens:
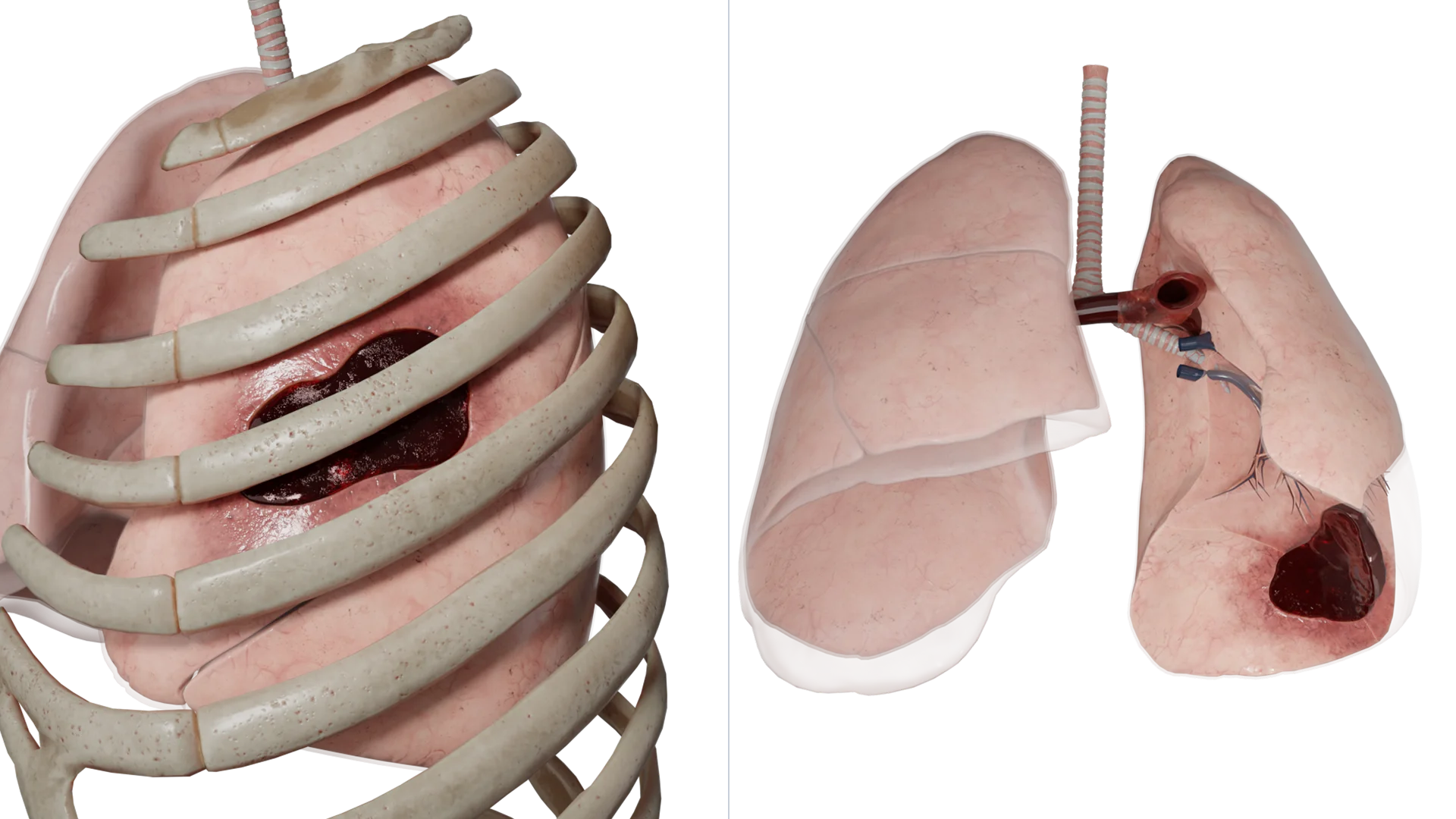

By the presence of bleeding:
By the presence of complications hemothorax comes:
Internal bleeding in trauma leads to accumulation of blood in the pleural cavity, which further causes compression (compression) of the lung on the affected side, and with continued bleeding – to displacement of the mediastinum to the healthy side and compression of the healthy lung. Because of this, there is a decrease in respiratory volume and respiratory surface of the lung and, as a consequence, impaired gas exchange. Also displacement of the mediastinum with compression of hollow veins and pulmonary vessels has an unfavorable effect on hemodynamics. The clinic of acute respiratory and cardiac failure appears.
Symptoms and signs may be due to the etiology of the hemothorax, such as pain from rib fracture. Clues to the diagnosis come from the patient’s medical history.
The course may be asymptomatic at low volumes of single blood loss. Or have a latent period (imaginary well-being) at a low rate of blood loss or overexpressed compensatory capabilities of the body. May have nonspecific symptoms in relation to the pathology: pain or discomfort in the chest, cough, dyspnea.
The most common manifestations include signs of tachypnea, tachycardia, and hypotension. The skin and mucous membranes of such patients are pale or cyanotic. In severe course of the process is characterized by a frequent thready pulse, suffocation in the supine position, lack of consciousness or loss of consciousness when the patient is verticalized.
When infection occurs, there is a clinic of general inflammatory syndrome: hyperthermia, fever, chills, pain on the affected side, cough, asthenic syndrome and so on.
Fibrothorax may be asymptomatic, with marked compression of the lung, the clinic of chronic respiratory failure joins.

Trauma (even minor), malignant neoplasm, or recent medical intervention are most commonly reported.
Carefully looking for any signs of trauma such as bruising or soreness of the ribs/chest wall is a must.
Physical examination findings are usually consistent with the clinic of any pleural effusion.
On percussion of the affected half of the chest there may be a shortening of the percussion sound, the upper border of fluid, if there is no pneumothorax, may form the Damoiseau line. The heart boundaries may be displaced to the healthy side.
At auscultation of the lungs is determined by weakening of respiratory noises or their absence.
The clarity of the physical signs of fluid depends on the magnitude of the hemothorax.

Routine method of diagnosing hemothorax. It is a relatively quick and inexpensive method of investigation. It can provide information about the underlying etiology, concomitant complications (e.g. rib fracture), lung collapse, mediastinal displacement, etc., as well as the underlying cause. Hemothorax can usually be visualized when the volume of blood in the pleural cavity is greater than 500 mL in adults. In this case, the darkening on the radiograph occupies the pleural sinuses. In a medium hemothorax, the level of darkening reaches the angle of the scapula. In a large hemothorax, blood occupies almost the entire pleural cavity. However, early hemothorax may not be seen on radiographs if images are obtained in the supine position (typical of trauma).
This method does not have good screening capabilities in closed chest trauma, with a sensitivity of up to 50%. If significant clinical manifestations are present, the sensitivity increases only to 75%.

It has high specificity and allows to detect pleural fluid in the volume of 100 ml with an accuracy of 100%, and from 20 ml – with an accuracy of 75% (in adults). Ultrasound is an alternative method when computerized or magnetic resonance imaging (CT, MRI) is not possible. However, the study is difficult in subcutaneous emphysema and obesity.
One disadvantage of ultrasound is that it cannot provide confirmation of the etiology of hemothorax and associated information about other thoracic structures (e.g., aortic dissection) to the same extent as CT/MRI.
The methods have the highest diagnostic sensitivity in relation to hemothorax. Since they allow to characterize in 3D space both the presence of fluid and its localization, for example, in case of delimited hemothorax. The disadvantages are high cost, ionizing radiation in CT, the need to transport the patient to a specialized department, and the availability of devices is not in every clinic.
Diagnostic puncture or drainage of the pleural cavity to visualize the aspirate. After collection of the contents, a Rouvelois-Gregoire test may be performed to determine whether bleeding is ongoing or has occurred.
Hospitalization in the surgical department under the supervision of a thoracic surgeon.

Hemothorax of less than 260-300 ml with separation (divergence) of pleural sheets 1.5-2 cm in adults usually resolves without complications and additional intervention. If the patient is stable in this situation, conservative treatment is possible with dynamic observation, serial hemoglobin analysis, repeated radiography or ultrasound to ensure that the hemothorax does not progress. Conservative treatments include symptomatic (including oxygen therapy), hemostatic, hemostatic, hemotransfusion, antiaggregant, immunocorrective, and antibiotic therapy.
Indications for blood evacuation (thoracocentesis and drainage) are progressive clinical course of hemothorax, blood volume more than 300-500 ml in adults and separation of pleural sheets more than 3 cm.
Thoracoscopy with blood removal for urgent indications is performed in the first 24-72 hours after trauma in the stable condition of the patient for residual, recurrent or coagulated hemothorax, preventing lung expansion, as well as for the prevention of infection.

The presence of 1500 ml or more of blood in the pleural cavity or dynamic inflow of more than 250 ml of blood hourly for three consecutive hours through the drainage tube are indications for emergency surgical intervention (thoracoscopy, thoracotomy). Vascular ligations, suturing of lung and/or pericardial wounds, removal of accumulated blood, etc. are performed.
1. What is the danger of blood pooling in the pleural cavity?
2. What complications can occur with hemothorax?
3. When is surgical intervention required?
4. How can complications of hemothorax be prevented?
List of Sources
1.
VOKA Catalog.
https://catalog.voka.io/
2.
Patel NJ, Dultz L, Ladhani HA, Cullinane DC, Klein E, McNickle AG, Bugaev N, Fraser DR, Kartiko S, Dodgion C, Pappas PA, Kim D, Cantrell S, Como JJ, Kasotakis G. Management of simple and retained hemothorax: A practice management guideline from the Eastern Association for the Surgery of Trauma. Am J Surg. 2021 May;221(5):873-884. doi: 10.1016/j.amjsurg.2020.11.032. Epub 2020 Nov 17. PMID: 33487403.
3.
Васильев И.В., Ли В.Ф., Скороход А.А., Соколович Е.Г., Яблонский П.К., Клинические рекомендации по тактике лечения больных легочным кровотечением.
4.
Коржева И. Ю. Лёгочные кровотечения. Комплексная диагностика и лечение. Автореферат диссертации на соискание ученой степени доктора медицинских наук. Москва. – 2012. – С. 3-4.
5.
Walker S, Hallifax R, Ricciardi S, Fitzgerald D, Keijzers M, Lauk O, Petersen J, Bertolaccini L, Bodtger U, Clive A, Elia S, Froudarakis M, Janssen J, Lee YCG, Licht P, Massard G, Nagavci B, Neudecker J, Roessner E, Van Schil P, Waller D, Walles T, Cardillo G, Maskell N, Rahman N. Joint ERS/EACTS/ESTS clinical practice guidelines on adults with spontaneous pneumothorax. Eur Respir J. 2024 May 28;63(5):2300797. doi: 10.1183/13993003.00797-2023. PMID: 38806203.
6.
Choi WI. Pneumothorax. Tuberc Respir Dis (Seoul). 2014 Mar;76(3):99-104. doi: 10.4046/trd.2014.76.3.99. Epub 2014 Mar 29. PMID: 24734096; PMCID: PMC3982243.
Summarize article with AI
Choose your preferable AI assistant:
Link successfully copied to clipboard
Thank you!
Your message is sent!
Our experts will contact you shortly. If you have any additional questions, please contact us at info@voka.io