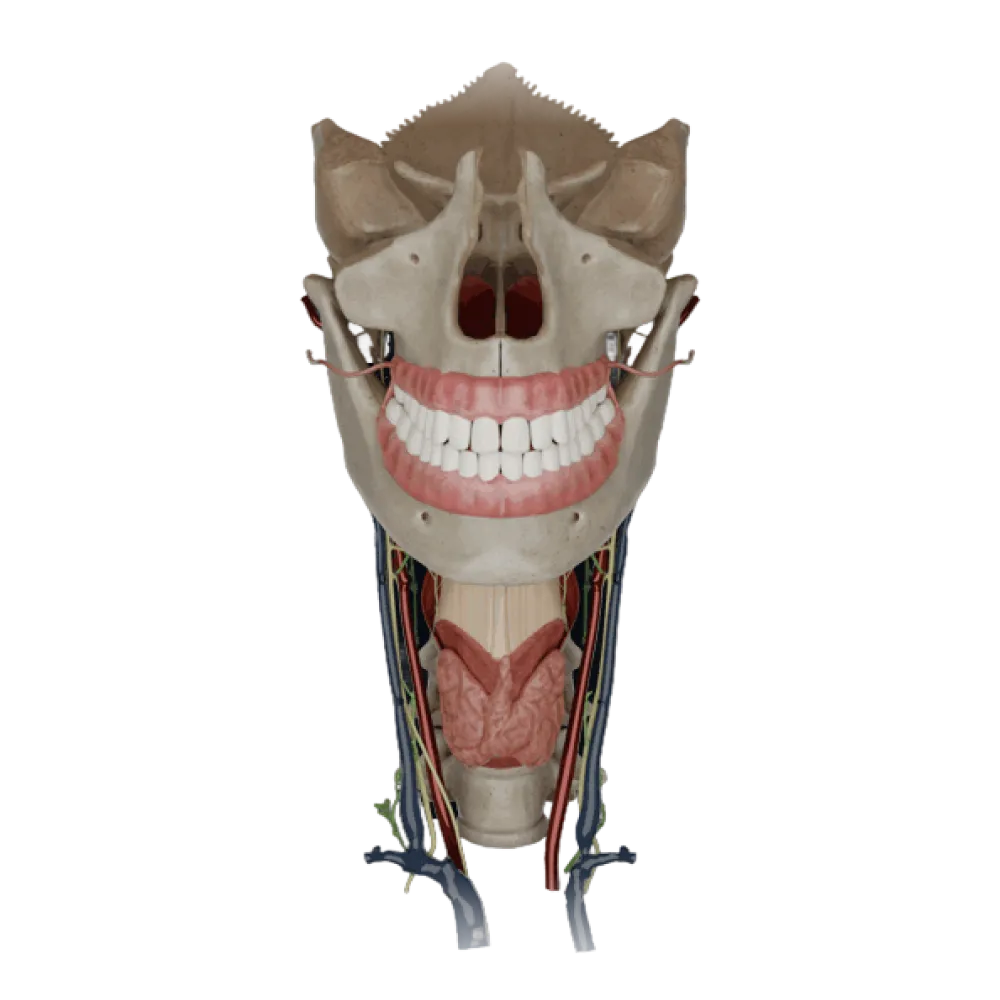
Thyroid and parathyroid glands anatomy test
Check your knowledge of thyroid and parathyroid glands anatomy. The test covers their topography, blood supply, innervation, and lymphatic drainage.
1/20
bold
text
1. At what level of the respiratory tract structures is the isthmus of the thyroid gland normally located?
-
Cricoid cartilage and the first tracheal ring
The isthmus of the thyroid gland is usually located anterior to the second to fourth tracheal rings, sometimes reaching the first ring or the cricoid cartilage.
-
V–VII tracheal rings
The isthmus of the thyroid gland is usually located anterior to the second to fourth tracheal rings, sometimes reaching the first ring or the cricoid cartilage.
-
II–IV tracheal rings
The isthmus of the thyroid gland is usually located anterior to the second to fourth tracheal rings, sometimes reaching the first ring or the cricoid cartilage.
-
Thyroid cartilage of the larynx
The isthmus of the thyroid gland is usually located anterior to the second to fourth tracheal rings, sometimes reaching the first ring or the cricoid cartilage.
-
I find it difficult to answer
The isthmus of the thyroid gland is usually located anterior to the second to fourth tracheal rings, sometimes reaching the first ring or the cricoid cartilage.
2. Branching from which blood vessel is the superior thyroid artery (a. thyroidea superior)?
-
External carotid artery
The superior thyroid artery is the first branch of the external carotid artery, branching from it immediately above the bifurcation of the common carotid artery.
-
Thyrocervical trunk
The superior thyroid artery is the first branch of the external carotid artery, branching from it immediately above the bifurcation of the common carotid artery.
-
Internal carotid artery
The superior thyroid artery is the first branch of the external carotid artery, branching from it immediately above the bifurcation of the common carotid artery.
-
Brachiocephalic trunk
The superior thyroid artery is the first branch of the external carotid artery, branching from it immediately above the bifurcation of the common carotid artery.
-
I find it difficult to answer
The superior thyroid artery is the first branch of the external carotid artery, branching from it immediately above the bifurcation of the common carotid artery.
3. From which vascular formation does the inferior thyroid artery (a. thyroidea inferior) typically originate?
-
External carotid artery
The inferior thyroid artery branches from the thyrocervical trunk (truncus thyrocervicalis), which is a branch of the subclavian artery.
-
Costocervical trunk
The inferior thyroid artery branches from the thyrocervical trunk (truncus thyrocervicalis), which is a branch of the subclavian artery.
-
Subclavian artery
The inferior thyroid artery branches from the thyrocervical trunk (truncus thyrocervicalis), which is a branch of the subclavian artery.
-
Thyrocervical trunk
The inferior thyroid artery branches from the thyrocervical trunk (truncus thyrocervicalis), which is a branch of the subclavian artery.
-
I find it difficult to answer
The inferior thyroid artery branches from the thyrocervical trunk (truncus thyrocervicalis), which is a branch of the subclavian artery.
4. Into which blood vessel do the middle thyroid veins (vv. thyroideae mediae) drain?
-
Into the brachiocephalic vein
The middle and superior thyroid veins drain into the internal jugular vein, while the inferior veins more often flow into the brachiocephalic veins.
-
Into the external jugular vein.
The middle and superior thyroid veins drain into the internal jugular vein, while the inferior veins more often flow into the brachiocephalic veins.
-
Into the anterior jugular vein
The middle and superior thyroid veins drain into the internal jugular vein, while the inferior veins more often flow into the brachiocephalic veins.
-
Into the internal jugular vein.
The middle and superior thyroid veins drain into the internal jugular vein, while the inferior veins more often flow into the brachiocephalic veins.
-
I find it difficult to answer
The middle and superior thyroid veins drain into the internal jugular vein, while the inferior veins more often flow into the brachiocephalic veins.
5. Which fascia of the neck (according to V. N. Shevkunenko's classification) forms the outer capsule (fascia thyroidea) of the thyroid gland?
-
Superficial fascia of the neck (first)
The thyroid gland is covered by the visceral layer of the endocervical fascia (fascia endocervicalis), forming its fascial sheath.
-
Endocervical fascia, visceral layer (fourth)
The thyroid gland is covered by the visceral layer of the endocervical fascia (fascia endocervicalis), forming its fascial sheath.
-
Superficial layer of the deep cervical fascia (second)
The thyroid gland is covered by the visceral layer of the endocervical fascia (fascia endocervicalis), forming its fascial sheath.
-
Prevertebral fascia (fifth)
The thyroid gland is covered by the visceral layer of the endocervical fascia (fascia endocervicalis), forming its fascial sheath.
-
I find it difficult to answer
The thyroid gland is covered by the visceral layer of the endocervical fascia (fascia endocervicalis), forming its fascial sheath.
6. Where are the parathyroid glands normally located in relation to the capsules of the thyroid gland?
-
Outside the fascial sheath of the gland
The parathyroid glands are located in the loose connective tissue between the fibrous capsule, tightly fused with the parenchyma, and the external fascial sheath of the thyroid gland.
-
Within the parenchyma of the thyroid gland
The parathyroid glands are located in the loose connective tissue between the fibrous capsule, tightly fused with the parenchyma, and the external fascial sheath of the thyroid gland.
-
Between the true fibrous capsule and the fascial sheath
The parathyroid glands are located in the loose connective tissue between the fibrous capsule, tightly fused with the parenchyma, and the external fascial sheath of the thyroid gland.
-
Beneath the true fibrous capsule, penetrating into the lobules
The parathyroid glands are located in the loose connective tissue between the fibrous capsule, tightly fused with the parenchyma, and the external fascial sheath of the thyroid gland.
-
I find it difficult to answer
The parathyroid glands are located in the loose connective tissue between the fibrous capsule, tightly fused with the parenchyma, and the external fascial sheath of the thyroid gland.
7. From what source are the parathyroid glands predominantly vascularized?
-
From branches of the superior thyroid arteries
The blood supply of both the superior and inferior parathyroid glands is mainly provided by branches of the inferior thyroid arteries.
-
From branches of the inferior thyroid arteries
The blood supply of both the superior and inferior parathyroid glands is mainly provided by branches of the inferior thyroid arteries.
-
From the thyroidea ima artery
The blood supply of both the superior and inferior parathyroid glands is mainly provided by branches of the inferior thyroid arteries.
-
From the laryngeal arteries
The blood supply of both the superior and inferior parathyroid glands is mainly provided by branches of the inferior thyroid arteries.
-
I find it difficult to answer
The blood supply of both the superior and inferior parathyroid glands is mainly provided by branches of the inferior thyroid arteries.
8. Which nerve passes in the tracheoesophageal groove and is closely adjacent to the posterior surface of the thyroid gland lobes?
-
Superior laryngeal nerve.
The recurrent laryngeal nerve (branch of the vagus nerve) ascends to the larynx in the tracheoesophageal groove, lying directly adjacent to the posterior surface of the thyroid gland, and crossing the inferior thyroid artery.
-
Accessory nerve
The recurrent laryngeal nerve (branch of the vagus nerve) ascends to the larynx in the tracheoesophageal groove, lying directly adjacent to the posterior surface of the thyroid gland, and crossing the inferior thyroid artery.
-
Hypoglossal nerve
The recurrent laryngeal nerve (branch of the vagus nerve) ascends to the larynx in the tracheoesophageal groove, lying directly adjacent to the posterior surface of the thyroid gland, and crossing the inferior thyroid artery.
-
Recurrent laryngeal nerve.
The recurrent laryngeal nerve (branch of the vagus nerve) ascends to the larynx in the tracheoesophageal groove, lying directly adjacent to the posterior surface of the thyroid gland, and crossing the inferior thyroid artery.
-
I find it difficult to answer
The recurrent laryngeal nerve (branch of the vagus nerve) ascends to the larynx in the tracheoesophageal groove, lying directly adjacent to the posterior surface of the thyroid gland, and crossing the inferior thyroid artery.
9. Which neck muscle does NOT adjoin the anterior surface of the thyroid gland?
-
Digastric muscle
Anteriorly, the thyroid gland is covered by muscles lying below the hyoid bone: mm. sternohyoideus, sternothyroideus, omohyoideus. The digastric muscle lies above.
-
Sternothyroid muscle
Anteriorly, the thyroid gland is covered by muscles lying below the hyoid bone: mm. sternohyoideus, sternothyroideus, omohyoideus. The digastric muscle lies above.
-
Sternohyoid muscle.
Anteriorly, the thyroid gland is covered by muscles lying below the hyoid bone: mm. sternohyoideus, sternothyroideus, omohyoideus. The digastric muscle lies above.
-
Omohyoid muscle
Anteriorly, the thyroid gland is covered by muscles lying below the hyoid bone: mm. sternohyoideus, sternothyroideus, omohyoideus. The digastric muscle lies above.
-
I find it difficult to answer
Anteriorly, the thyroid gland is covered by muscles lying below the hyoid bone: mm. sternohyoideus, sternothyroideus, omohyoideus. The digastric muscle lies above.
10. How often (approximately) does the pyramidal lobe (lobus pyramidalis) of the thyroid gland occur in the population?
-
No more than 5%
The pyramidal lobe is a remnant of the thyroglossal duct and occurs as an inconstant structure in 30-50% of people.
-
Approximately 90-95%
The pyramidal lobe is a remnant of the thyroglossal duct and occurs as an inconstant structure in 30-50% of people.
-
100% (is a constant structure)
The pyramidal lobe is a remnant of the thyroglossal duct and occurs as an inconstant structure in 30-50% of people.
-
Approximately 30-50%
The pyramidal lobe is a remnant of the thyroglossal duct and occurs as an inconstant structure in 30-50% of people.
-
I find it difficult to answer
The pyramidal lobe is a remnant of the thyroglossal duct and occurs as an inconstant structure in 30-50% of people.
11. Where does lymphatic drainage from the isthmus and lower parts of the thyroid gland primarily occur?
-
To the retropharyngeal lymph nodes
Lymph from the lower parts of the gland and the isthmus drains into the nodi lymphatici prelaryngeales, pretracheales, and paratracheales.
-
To the prelaryngeal and pretracheal lymph nodes
Lymph from the lower parts of the gland and the isthmus drains into the nodi lymphatici prelaryngeales, pretracheales, and paratracheales.
-
To the submandibular lymph nodes
Lymph from the lower parts of the gland and the isthmus drains into the nodi lymphatici prelaryngeales, pretracheales, and paratracheales.
-
To the submental lymph nodes
Lymph from the lower parts of the gland and the isthmus drains into the nodi lymphatici prelaryngeales, pretracheales, and paratracheales.
-
I find it difficult to answer
Lymph from the lower parts of the gland and the isthmus drains into the nodi lymphatici prelaryngeales, pretracheales, and paratracheales.
12. From where does the thyroidea ima artery (a. thyroidea ima), found in 10-12% of people, most often originate?
-
From the brachiocephalic trunk or the aortic arch
Arteria thyroidea ima (Neubauer's artery) most often originates from the brachiocephalic trunk (truncus brachiocephalicus) or directly from the aortic arch and ascends to the isthmus of the gland.
-
From the internal thoracic artery
Arteria thyroidea ima (Neubauer's artery) most often originates from the brachiocephalic trunk (truncus brachiocephalicus) or directly from the aortic arch and ascends to the isthmus of the gland.
-
From the external carotid artery
Arteria thyroidea ima (Neubauer's artery) most often originates from the brachiocephalic trunk (truncus brachiocephalicus) or directly from the aortic arch and ascends to the isthmus of the gland.
-
From the vertebral artery
Arteria thyroidea ima (Neubauer's artery) most often originates from the brachiocephalic trunk (truncus brachiocephalicus) or directly from the aortic arch and ascends to the isthmus of the gland.
-
I find it difficult to answer
Arteria thyroidea ima (Neubauer's artery) most often originates from the brachiocephalic trunk (truncus brachiocephalicus) or directly from the aortic arch and ascends to the isthmus of the gland.
13. Which structures innervate the thyroid gland with sympathetic fibers?
-
Thoracic nodes of the sympathetic trunk
Sympathetic innervation is provided by postganglionic fibers from the upper, middle, and lower (stellate) cervical ganglia of the sympathetic trunk.
-
Cervical nodes of the sympathetic trunk
Sympathetic innervation is provided by postganglionic fibers from the upper, middle, and lower (stellate) cervical ganglia of the sympathetic trunk.
-
Nodes of the celiac plexus
Sympathetic innervation is provided by postganglionic fibers from the upper, middle, and lower (stellate) cervical ganglia of the sympathetic trunk.
-
Pterygopalatine and otic nodes
Sympathetic innervation is provided by postganglionic fibers from the upper, middle, and lower (stellate) cervical ganglia of the sympathetic trunk.
-
I find it difficult to answer
Sympathetic innervation is provided by postganglionic fibers from the upper, middle, and lower (stellate) cervical ganglia of the sympathetic trunk.
14. With which artery does the external branch of the superior laryngeal nerve come into close contact when approaching the superior pole of the thyroid gland?
-
With the inferior thyroid artery
The external branch of the superior laryngeal nerve (ramus externus n. laryngei superioris) descends along the superior thyroid artery to the superior pole of the gland, requiring caution when ligating the vessel.
-
With the thyroidea ima artery
The external branch of the superior laryngeal nerve (ramus externus n. laryngei superioris) descends along the superior thyroid artery to the superior pole of the gland, requiring caution when ligating the vessel.
-
With the superior thyroid artery
The external branch of the superior laryngeal nerve (ramus externus n. laryngei superioris) descends along the superior thyroid artery to the superior pole of the gland, requiring caution when ligating the vessel.
-
With the ascending pharyngeal artery
The external branch of the superior laryngeal nerve (ramus externus n. laryngei superioris) descends along the superior thyroid artery to the superior pole of the gland, requiring caution when ligating the vessel.
-
I find it difficult to answer
The external branch of the superior laryngeal nerve (ramus externus n. laryngei superioris) descends along the superior thyroid artery to the superior pole of the gland, requiring caution when ligating the vessel.
15. Where do the inferior thyroid veins (vv. thyroideae inferiores) drain?
-
Into the brachiocephalic veins
The inferior thyroid veins, often forming an unpaired venous plexus (plexus thyroideus impar), drain into the left and right brachiocephalic veins.
-
Into the azygos vein.
The inferior thyroid veins, often forming an unpaired venous plexus (plexus thyroideus impar), drain into the left and right brachiocephalic veins.
-
Into the superior vena cava
The inferior thyroid veins, often forming an unpaired venous plexus (plexus thyroideus impar), drain into the left and right brachiocephalic veins.
-
Into the internal jugular vein.
The inferior thyroid veins, often forming an unpaired venous plexus (plexus thyroideus impar), drain into the left and right brachiocephalic veins.
-
I find it difficult to answer
The inferior thyroid veins, often forming an unpaired venous plexus (plexus thyroideus impar), drain into the left and right brachiocephalic veins.
16. To what does the posteromedial surface of the lateral lobes of the thyroid gland adjoin?
-
To the prevertebral fascia and long muscles of the neck
The posteromedial surface of the lobes adjoins the organs of the neck: larynx, trachea, pharynx, and esophagus, as well as the recurrent laryngeal nerve.
-
To the larynx, trachea, pharynx, and esophagus
The posteromedial surface of the lobes adjoins the organs of the neck: larynx, trachea, pharynx, and esophagus, as well as the recurrent laryngeal nerve.
-
To the carotid artery and jugular vein
The posteromedial surface of the lobes adjoins the organs of the neck: larynx, trachea, pharynx, and esophagus, as well as the recurrent laryngeal nerve.
-
To the sternocleidomastoid muscle
The posteromedial surface of the lobes adjoins the organs of the neck: larynx, trachea, pharynx, and esophagus, as well as the recurrent laryngeal nerve.
-
I find it difficult to answer
The posteromedial surface of the lobes adjoins the organs of the neck: larynx, trachea, pharynx, and esophagus, as well as the recurrent laryngeal nerve.
17. What anatomical structure is located laterally (outside) to the lateral lobes of the thyroid gland?
-
Trachea
Lateral to the lateral lobes is the cervical neurovascular bundle (common carotid artery, internal jugular vein, vagus nerve).
-
Esophagus
Lateral to the lateral lobes is the cervical neurovascular bundle (common carotid artery, internal jugular vein, vagus nerve).
-
Prevertebral connective tissue
Lateral to the lateral lobes is the cervical neurovascular bundle (common carotid artery, internal jugular vein, vagus nerve).
-
Cervical neurovascular bundle
Lateral to the lateral lobes is the cervical neurovascular bundle (common carotid artery, internal jugular vein, vagus nerve).
-
I find it difficult to answer
Lateral to the lateral lobes is the cervical neurovascular bundle (common carotid artery, internal jugular vein, vagus nerve).
18. How many parathyroid glands are most commonly found in a person?
-
Two.
Normally, a person most often has four parathyroid glands: two superior and two inferior, although their number can vary.
-
Four.
Normally, a person most often has four parathyroid glands: two superior and two inferior, although their number can vary.
-
Three.
Normally, a person most often has four parathyroid glands: two superior and two inferior, although their number can vary.
-
Six
Normally, a person most often has four parathyroid glands: two superior and two inferior, although their number can vary.
-
I find it difficult to answer
Normally, a person most often has four parathyroid glands: two superior and two inferior, although their number can vary.
19. What is the suspensory ligament of the thyroid gland (Berry's ligament)?
-
Remnant of the thyroglossal duct
Berry's ligament (ligamentum suspensorium glandulae thyroideae) is formed by the visceral layer of the cervical fascia and securely fixes the gland to the cricoid cartilage and trachea.
-
Ligament connecting the isthmus of the gland to the hyoid bone
Berry's ligament (ligamentum suspensorium glandulae thyroideae) is formed by the visceral layer of the cervical fascia and securely fixes the gland to the cricoid cartilage and trachea.
-
Thickening of the cervical fascia that secures the capsule of the gland to the cricoid cartilage and tracheal rings
Berry's ligament (ligamentum suspensorium glandulae thyroideae) is formed by the visceral layer of the cervical fascia and securely fixes the gland to the cricoid cartilage and trachea.
-
Fibrous band between the neurovascular bundle of the neck and the lobes of the gland
Berry's ligament (ligamentum suspensorium glandulae thyroideae) is formed by the visceral layer of the cervical fascia and securely fixes the gland to the cricoid cartilage and trachea.
-
I find it difficult to answer
Berry's ligament (ligamentum suspensorium glandulae thyroideae) is formed by the visceral layer of the cervical fascia and securely fixes the gland to the cricoid cartilage and trachea.
20. What is the typical relationship of the crossing of the inferior thyroid artery and the recurrent laryngeal nerve?
-
The nerve can pass both anteriorly and posteriorly to the artery or between its branches
The relationships of the inferior thyroid artery and the recurrent laryngeal nerve are highly variable: the nerve may pass anteriorly, posteriorly to the vessel, or penetrate between its branches.
-
The artery always passes anteriorly to the nerve
The relationships of the inferior thyroid artery and the recurrent laryngeal nerve are highly variable: the nerve may pass anteriorly, posteriorly to the vessel, or penetrate between its branches.
-
The artery always passes posteriorly to the nerve
The relationships of the inferior thyroid artery and the recurrent laryngeal nerve are highly variable: the nerve may pass anteriorly, posteriorly to the vessel, or penetrate between its branches.
-
These structures never cross each other
The relationships of the inferior thyroid artery and the recurrent laryngeal nerve are highly variable: the nerve may pass anteriorly, posteriorly to the vessel, or penetrate between its branches.
-
I find it difficult to answer
The relationships of the inferior thyroid artery and the recurrent laryngeal nerve are highly variable: the nerve may pass anteriorly, posteriorly to the vessel, or penetrate between its branches.
Retake this quiz?
Your current progress will be reset.